Autoclaves are a critical part of effective infection control in the dental office, with a plethora of autoclaves to choose from. If you are replacing an existing autoclave, and your needs are unchanged, you may be happy to purchase the same or a similar one. Whether you are looking to purchase your next autoclave, an additional autoclave, or your first autoclave, there are a number of considerations.
With that in mind, here are ten steps in choosing your next autoclave that will help you make a good decision:
Step 1: Volume and types of instruments
First consider the instruments being sterilized. How many instruments are/will you use per day, and how often will they be needed? What types of instruments? How many handpieces do you use daily? Do you have any instruments you are keeping or purchasing that require a dedicated cycle?
Step 2: Gravity displacement or vacuum autoclave
Gravity displacement (Class N) and pre-vacuum (Class B) autoclaves are available. A third type, the Class S, has varying features and indications provided by the manufacturer for a specific autoclave. (EN 13060) Gravity displacement autoclaves are the simplest, relying on gravity to push air out through exit valves at the chamber’s base when steam enters to displace the air. Pre-vacuum autoclaves contain a vacuum pump that creates negative pressure and forces steam in. This results in more effective air removal than gravity displacement, particularly for wrapped loads and devices with lumens, e.g., handpieces. For autoclaves with a post-vacuum, drying efficiency is also improved.
Which type do you want or need? It depends. It is essential to know the regulations and standards where you practice! In Europe, standard EN 13060 recommends vacuum autoclaves for medical devices. Depending on your location, gravity displacement may only be recommended (or allowed) for unwrapped loads and solid instruments (i.e., no hollows/lumens) and a pre-vacuum autoclave for packaged loads, solid and lumened instruments. In another location, pre-vacuum autoclaves may be mandated for handpieces. In yet another, any type of autoclave may be recommended, while unwrapped/unpackaged loads are not allowed or are strongly discouraged.
Note that autoclaves are validated by the manufacturer for the loads and cycles indicated in the instructions for use (IFU), for wrapped and unwrapped loads as appropriate. Medical device approval by the relevant authority occurs for each location
Step 3: Chamber Size and load capacity
For small steam sterilizers used in the dental clinic chamber size can be up to 60 liters. The internal dimensions of the cylinder itself and configuration of trays and racks within it also vary, influencing the loads that can be accommodated. A chamber large enough and configured to accommodate the instrument loads you need, but not excessive, is ideal. Consider whether two smaller or one large autoclave would be best.
Step 4: Cycle times
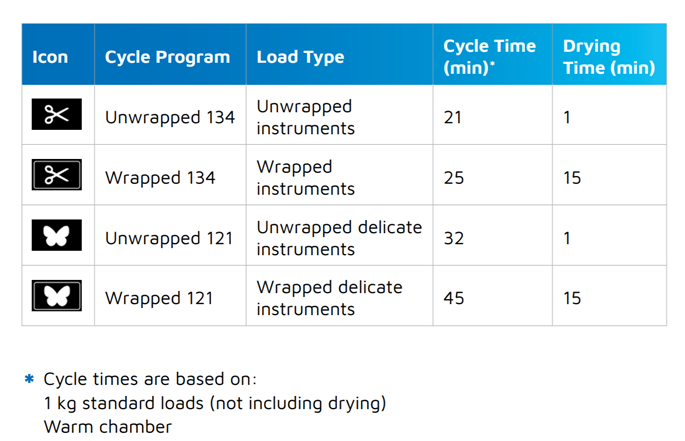
Cycle times vary by autoclave type and cycle parameters, as do warm-up and cooling times. Consider each stage in the process. If an autoclave requires a pre-heat phase, that needs to be added in, as does drying time. Quicker cycles do result in more rapid reprocessing and autoclave availability for subsequent loads.
Step 5: Available space
In a previous article we discuss the design of the instrument reprocessing room, as part of a clinic design. Designating and designing a space in advance can help to improve future performance and efficiency. The autoclave(s) must fit in the designated area in the reprocessing room, still allowing for set-down areas. We already considered load capacity and cycle times. If you have or anticipate a high throughput of instruments, it may be helpful to purchase two smaller autoclaves rather than one large one, depending on available space. This presents several potential advantages:
- Flexibility in processing smaller loads
- Smaller autoclaves require less energy than larger autoclaves
- Potential for simultaneous use/staggered loads
- Accommodation of anticipated growth
- You have a back-up! Instruments can be reprocessed uninterrupted (albeit fewer) should one autoclave be taken out of service.
Step 6: Manual or automated, ease-of-use
Manual autoclaves require time be spent on tasks that are effortlessly performed with automated autoclaves. For example, pre-programmed cycles remove the need to set sterilization parameters. Other examples include automated door-locking and release, a water-fill function, and digital documentation for the sterilization log. Nonetheless, manual autoclaves can be simple to use and are less expensive. For automated autoclaves, check there are sufficient pre-programmed cycles for your needs – note that an excessive number is not ideal either. Once you have narrowed down your choices, you may want to review IFUs.

Step 7: Accessories
Consider the availability and versatility of accessories such as racks for cassettes and trays for packaged instruments. These help to arrange instrument loads, and ensure sufficient space between packages, helping to avoid some errors and, e.g., wet packs. An incorporated printer may be included or USB ports for transfer of digital records.
Step 8: Sterilization logs
Autoclaves with digital output for record-keeping not only save time, they provide reliable records of autoclave performance and cycles for each load, for inclusion in the sterilization log. This is helpful in meeting requirements, and a best practice. In some cases, transmission of data occurs electronically.
Step 9: Maintenance Requirements, Warranties and Support
Make sure you know how much maintenance your autoclave will require, including replacement of consumables (e.g., gaskets, filters). Be clear on the warranty – the longer and more comprehensive, the better. Consider the reputation, expertise and quality of customer support from the autoclave company, and how quickly technical support would be available.
Step 10: Costs
Considering costs is inevitable and important. Are there additional installation costs? Are accessories included in the price? Assess initial and all ongoing costs, e.g., future maintenance, technical support and replacement parts. Smaller autoclaves are generally less expensive than larger autoclaves of the same quality – potentially another reason to consider a smaller autoclave initially and an additional one later for increased capacity.
In conclusion
When it comes to autoclaves, ‘one size does not fit all.’ There are choices galore and careful consideration and planning is invaluable. The distributor or local office for the autoclaves you are interested in can help you determine the best fit for you and your office. Investing time in these 10 steps can help you make the right investment when choosing a new autoclave for your dental office.
About Tuttnauer – We’re a one-stop shop for sterile dental processing
Tuttnauer provides end to end sterile processing solutions for dental clinics, including; advanced autoclave sterilizers, washer-disinfectors, indicators and sterile processing products. The T-Edge 23 autoclaves were explicitly developed for dental practices. They meet all your sterilization needs by creating cyclic parameters that accommodate with the most challenging loads, ensuring sterility and efficient drying, helping dentists achieve today’s challenging workloads and provide superior patient care, without risking cross patient contamination.
For further information and to inquire about purchasing the T-Edge 10 autoclave for your practice, visit the T-Edge page on our website.
Author: Fiona M. Collins
Dr. Collins graduated as a general dentist from the University of Glasgow and holds an MBA and an MA from Boston University. During her career, she has lived and worked in 5 countries and has given presentations internationally. Fiona is currently the ADA’s representative to the Association for the Advancement of Medical Instrumentation (AAMI), a member of the ADA, OSAP, a participant in infection control-related Standards working groups in AAMI, and a Fellow of the Pierre Fauchard Academy.